 In the case of left-sided colitis, the inflammation with redness and other irregularities in the gut’s lining are visible up to the splenic flexure (that “bend in the road”), but these signs disappear once the scope goes beyond that point. “When performing a colonoscopy, sometimes it’s like someone drew a sharp line in the colon and the disease stops at that line and doesn’t cross,” says Dr. During this procedure, a thin, fiber-optic camera is inserted into the anus and threaded into the rectum and colon to capture images of the lining. Diagnosing Left-Sided ColitisĪs with other forms of ulcerative colitis, left-sided colitis is usually diagnosed by a colonoscopy. 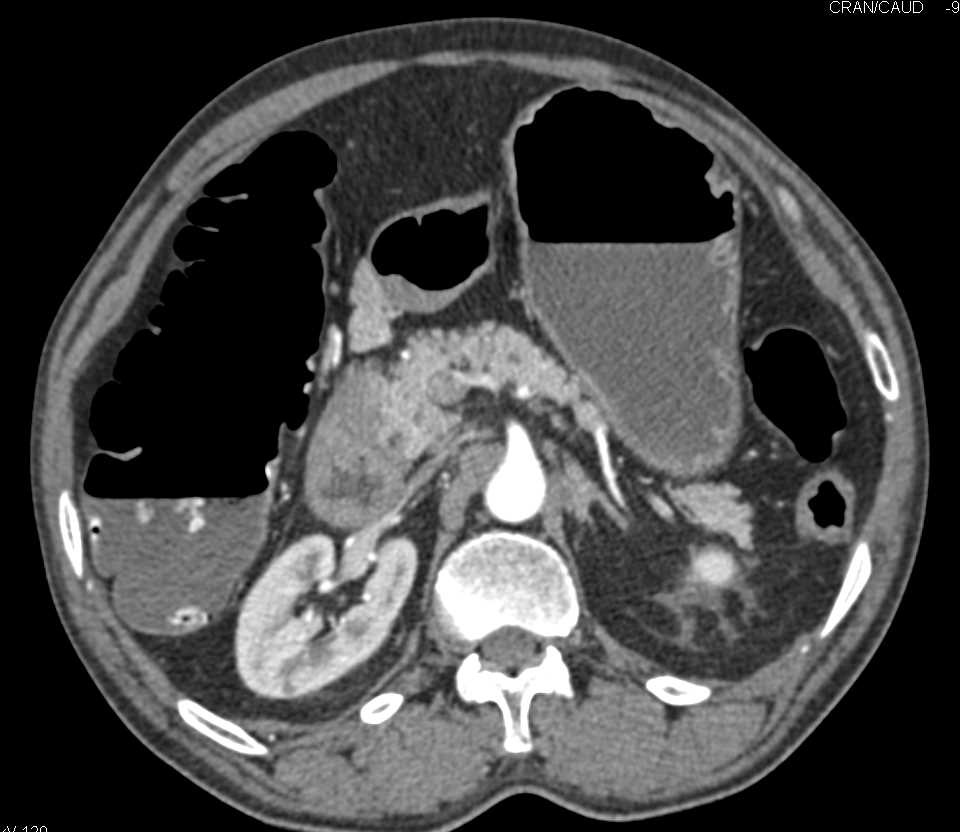
And in rare cases, if the inflammation becomes severe and is not treated, the colon can dilate and cause a condition called toxic megacolon. Katz, M.D., a professor of medicine at Case Western Reserve University School of Medicine in Cleveland, OH. 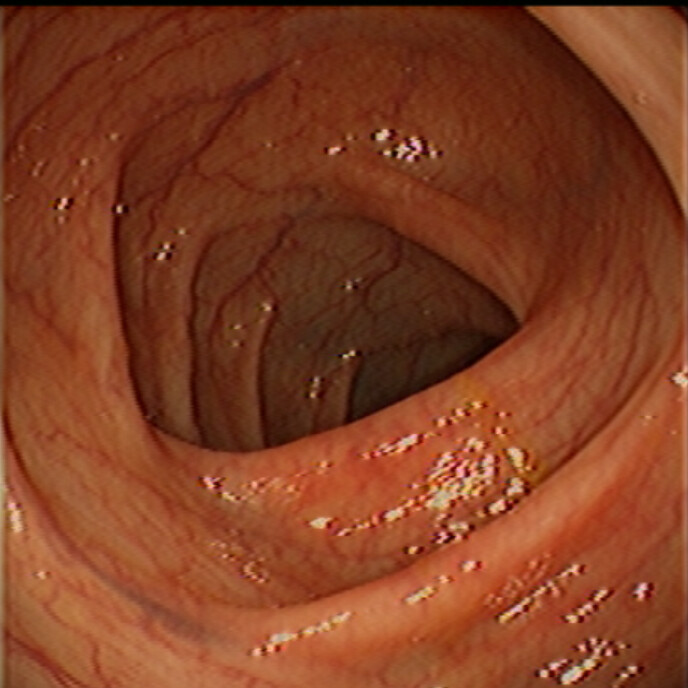
“If a patient has refractory (unmanageable) left-sided colitis, they can be quite ill, with debilitating bloody diarrhea leading to anemia, malnutrition, and weight loss,” says Jeffry A. It all depends on the degree of inflammation-not where the inflammation is located-as well as how well a person responds to medication. It’s logical to reason that if your UC is restricted to just the left side, it’s probably not as severe as UC that affects your entire colon. Other symptoms may include loss of appetite, weight loss, pain on the left side of the abdomen, and bloody diarrhea, according to the Crohn’s & Colitis Foundation. When people with left-sided UC do have constipation, they may find themselves spending a long time on the toilet or they may have to go many times in one day because the stool piles up in their colon. But colitis can alter bowel habits and there can be constipation as well.” Limketkai, “About 90% of individuals with UC, including left-sided, have diarrhea. Diarrhea is often cited as one of the most typical symptoms of any type of UC, according to Dr. You can’t talk about any kind of gut issue without first talking about irregular poop. And while it shares much in common with the more general UC crowd, left-sided colitis can have its own (fun!) set of side effects and symptoms. “About 34% of our ulcerative colitis patients have left-sided colitis-that’s not a small number.” Some research indicates that people who develop UC late in life (usually 60 years of age or older) are more likely to have left-sided colitis compared with younger individuals. You may never have heard of it, but “left-sided ulcerative colitis is not rare,” says Dr. If it goes beyond that-but not beyond the splenic flexure-that’s left-sided colitis,” says Berkeley Limketkai, M.D, Ph.D., an associate clinical professor at the David Geffen School of Medicine at the University of California, Los Angeles. “Ulcerative colitis starts in the rectum. As it travels down the left side of the abdomen toward your rectum, it’s known as the descending colon. Once it reaches the left side of your body, the colon bends downward-known as the splenic flexure. Then, going across the top of the inverted U, from right to left, is the middle colon (also called the transverse colon). 
On the right side of the abdomen is what’s referred to as the ascending colon, and it’s where digested food moves up from the small intestine. 
If you could see through your skin and straight into your abdomen, you’d see that the colon forms an upside-down “U” shape. In certain cases, it can be restricted to specific areas, which help define the four types of UC: Persistent diarrhea accompanied by abdominal pain and blood in the stoolĪs mentioned, UC can affect part of or the entire colon. People with UC battle a number of unpleasant symptoms, including: Race or ethnicity (white people have the highest risk of the disease) These include:Īge (while UC can occur at any age, it usually appears before age 30, with some people developing the disease after age 60) )įamily history (having a first-degree relative with the disease increases your risk) In addition, there are certain risk factors that make some people more likely to get UC, according to the Mayo Clinic. While the exact cause of UC is uncertain, research points to several potential variables in developing ulcerative colitis, including an abnormal immune response, genetics, your gut microbiome, and environmental influences. 
0 Comments
Leave a Reply. |

 RSS Feed
RSS Feed
